Diabetic Services
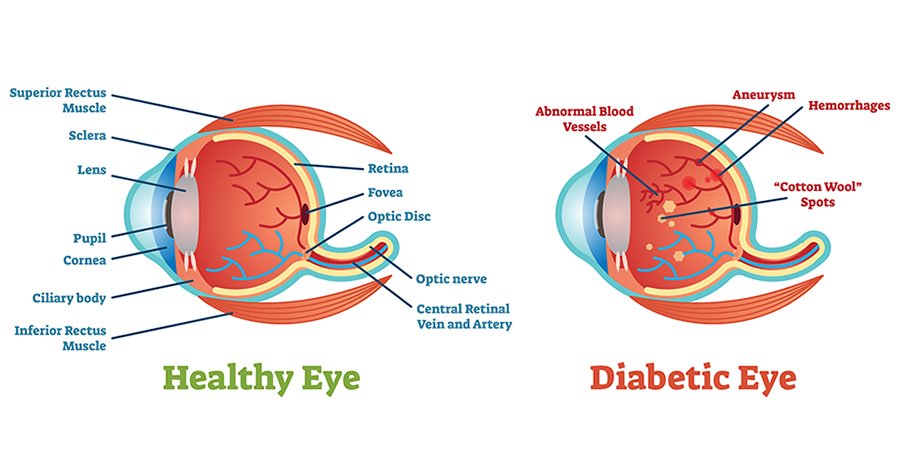
What is Daibetic Retinopathy?
Diabetic retinopathy is a diabetes-related eye condition that affects the retina, the light-sensitive tissue at the back of the eye. High blood sugar levels can damage the small blood vessels in the retina, causing them to leak, swell, or close off, leading to vision problems.
What Are the Causes of Diabetic Retinopathy?
The primary diabetic retinopathy causes include prolonged high blood sugar levels and associated conditions. The damage occurs in four stages:
- Mild Nonproliferative Retinopathy: Small bulges form in the blood vessels, causing leakage.
- Moderate Nonproliferative Retinopathy: Blood vessels swell and distort, further restricting blood flow.
- Severe Nonproliferative Retinopathy: Blocked blood vessels deprive the retina of oxygen, leading to new, fragile vessel growth.
- Proliferative Diabetic Retinopathy:
Advanced stage where new blood vessels form abnormally, leading to severe vision impairment.
Types of Diabetic Retinopathy
Proliferative Diabetic Retinopathy
The advanced form of the disease, where new, fragile blood vessels grow abnormally, leading to retinal detachment or hemorrhage, which can cause blindness.
Non Proliferative Diabetic Retinopathy
This is the early stage where tiny blood vessels swell and leak fluid into the retina, leading to mild vision problems.
Diabetic Retinopathy Risk Factors
Several factors increase the risk of developing diabetic retinopathy:
- Uncontrolled blood sugar levels
- High blood pressure and cholesterol
- Long-term diabetes (Type 1 or Type 2)
- Smoking and poor lifestyle habits
- Pregnancy-related diabetes (Gestational Diabetes)
How to Prevent Diabetic Retinopathy?
Preventing diabetic retinopathy involves maintaining overall eye health and managing diabetes effectively:
- Control blood sugar levels through a healthy diet and medication.
- Monitor blood pressure and cholesterol to reduce strain on blood vessels.
- Have regular eye exams to detect early changes in the retina.
- Quit smoking to improve circulation and eye health.
Stages of Diabetic Retinopathy
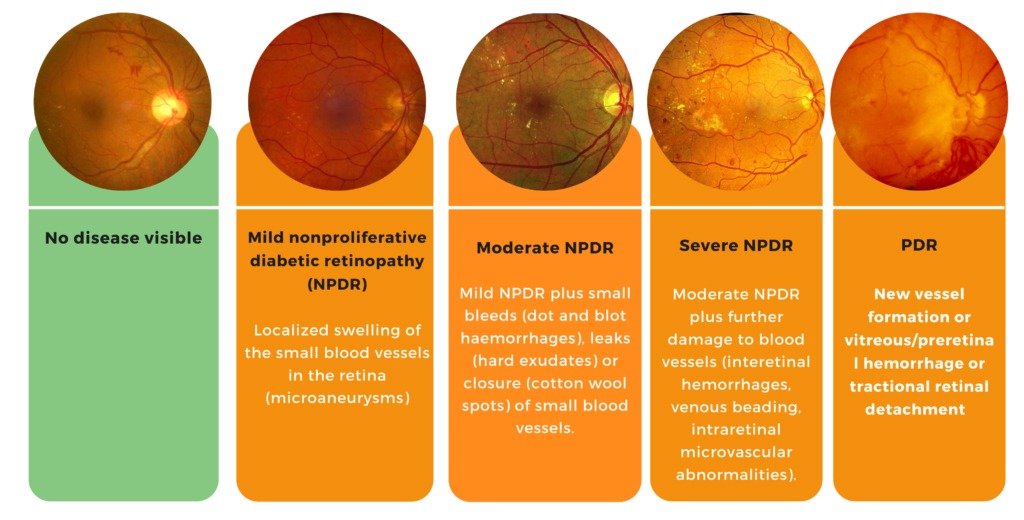
The diabetic retinopathy stages progress from mild to severe, requiring close monitoring and treatment:
- 1. Mild NPDR – Tiny swellings in the blood vessels, minor leakage.
- 2. Moderate NPDR – Blood vessel swelling restricts oxygen supply.
- 3. Severe NPDR – Widespread blockage leads to abnormal vessel growth.
- 4. Proliferative Diabetic Retinopathy (PDR) – Risk of hemorrhage and permanent vision loss.
Diabetic Retinopathy Diagnosis
- Visual Acuity Testing
A standard eye test to measure clarity of vision.
- Tonometry
Measures intraocular pressure to assess eye health.
- Pupil Dilation Exam
Drops are used to widen the pupil, allowing the doctor to examine the retina.
- Optical Coherence Tomography (OCT)
A detailed imaging test that detects retinal swelling and thickness changes.
- Fundus Fluorescein Angiography (FFA)
A dye is injected into the bloodstream to highlight blood vessel abnormalities in the retina.
Management of Diabetic Retinopathy
Effective management of diabetic retinopathy depends on the severity of the condition:
- Mild cases require regular monitoring and blood sugar control.
- Moderate to severe cases may require laser therapy or injections to reduce swelling.
- Advanced cases often require vitrectomy surgery to remove blood and prevent retinal detachment.
Proliferative Diabetic Retinopathy
Diabetic retinopathy occurs when high blood sugar levels cause damage to blood vessels in the retina. Diabetic retinopathy can progress to this more severe type, known as proliferative diabetic retinopathy when damaged blood vessels get blocked and new, abnormal blood vessels grow in the retina.
How can we help you?
Treatment Modalities
The goal of any treatment is to slow or stop the progression of the disease. In the early stages of non-proliferative diabetic retinopathy, regular monitoring may be the only treatment. Diet and exercise and controlling blood sugar levels can help control the progression of the disease.
Laser : If the disease advances, the blood vessels can leak blood and fluid into the retina, leading to macular edema. Laser treatment can stop this leakage. Focal laser photocoagulation involves using a laser to target a specific leaky vessel in the macula to keep macular edema from worsening. Widespread blood vessel growth in the retina, which occurs in proliferative diabetic retinopathy, can be treated by creating a pattern of scattered laser burns across the retina. This causes abnormal blood vessels to shrink and disappear.
Medical management: Injection of anti VEGF medication into the eye may help to reduce swelling of the macula, slowing vision loss and perhaps improving vision. Steroid injection into the eye is another option to reduce macular swelling.
Surgical management: Vitrectomy involves removing scar tissue and blood from the vitreous fluid of the eye.
Symptoms of Non Proliferative Diabetic Retinopathy
The symptoms of diabetic retinopathy often don’t appear until major damage occurs inside of the eye. They include
- Blurred vision/ loss of vision
- Seeing floaters or dark spots
- Difficulty seeing at night
- Difficulty distinguishing colors
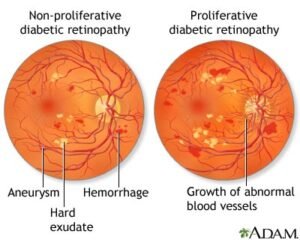
Proliferative Diabetic Retinopathy Risk Factors
- Diabetes: The longer a person has diabetes, the more likely he or she is to develop diabetic retinopathy, particularly if the diabetes is poorly controlled.
- Medical conditions:
other medical conditions like high blood pressure and high cholesterol increase the risk
- Pregnancy:
Pregnant women face a higher risk for developing diabetes and diabetic retinopathy.
- Heredity
- Sedentary lifestyle
- Diet
- Obesity
Proliferative Diabetic Retinopathy Diagnosis
Visual acuity testing:
This eye chart test measures a person’s vision
Tonometry:
This test measures pressure inside the eye.
Pupil dilation:
Drops placed on the eye’s surface widen the pupil, allowing a physician to examine the retina and optic nerve.
Proliferative Diabetic Retinopathy Prevention
You can’t always prevent diabetic retinopathy. If you are diagnosed with diabetes, it is important to do the following:
- Get regular eye exams and physical checkups.
- Keep your blood sugar, cholesterol, and blood pressure at healthy levels.
- Be mindful of any changes you may notice in your vision, and discuss them with your doctor.
- Stop smoking
- Regular exercise
Timely treatment and appropriate follow ups are important.
Proliferative Diabetic Retinopathy Complications
- Vitreous hemorrhage. The new blood vessels are fragile and may bleed into the eye. If the amount of bleeding is small, you might see only a few floaters. In severe cases, blood can fill the eye and cause reduced vision.
- Retinal detachment. The abnormal blood vessels can form scar tissue which can pull on the retina and cause retinal detachment.
- New blood vessels may grow in the front part of your eye and invade the drainage part of the eye, causing increased pressure in the eye. This pressure can damage the nerve that carries images from your eye to your brain.
Eventually, diabetic retinopathy, glaucoma or both can lead to complete vision loss.
Non Proliferative Diabetic Retinopathy
People with diabetes can have an eye disease called diabetic retinopathy. This is when high blood sugar levels cause damage to blood vessels in the retina. Diabetic retinopathy affects up to 80 percent of those who have had diabetes for 20 years or more. At least 90% of new cases could be reduced with proper treatment and monitoring of the eyes.
Proliferative Diabetic Retinopathy Treatment
The goal of any treatment is to slow or stop the progression of the disease. Diet and exercise and controlling blood sugar levels can help control the progression of the disease.
Laser :
Widespread blood vessel growth in the retina, which occurs in proliferative diabetic retinopathy, can be treated by creating a pattern of scattered laser burns across the retina. This causes abnormal blood vessels to shrink and disappear. With this procedure, some side vision may be lost in order to safeguard central vision
Medical management:
Injection of anti VEGF medication into the eye may be used in selected patients with bleeding into the eye.
Surgical management:
Vitrectomy involves removing scar tissue and blood from the vitreous fluid of the eye.
Symptoms of Non Proliferative Diabetic Retinopathy
The symptoms of diabetic retinopathy often don’t appear until major damage occurs inside of the eye. They include
- Blurred vision/ loss of vision
- Seeing floaters or dark spots
- Difficulty seeing at night
- Difficulty distinguishing colors
Non Proliferative Diabetic Retinopathy Risk Factors
- Diabetes: The longer a person has diabetes, the more likely he or she is to develop diabetic retinopathy, particularly if the diabetes is poorly controlled.
- Medical conditions: other medical conditions like high blood pressure and high cholesterol increase the risk
- Pregnancy
- Heredity
- Sedentary lifestyle
- Diet
Stages of Non Proliferative Diabetic Retinopathy
Comprehensive dilated eye exam:
It allows the doctor to check the retina for:
Changes to blood vessels or leaking blood vessels and new vessels
Fatty deposits
Swelling of the macula (Diabetic macular edema)
Changes in the lens
Damage to nerve tissue
Optical coherence tomography (OCT):
It uses light waves to produce images of the retina to assess the amount of fluid.
Fundus fluorescein angiography(FFA):
During this test, your doctor will inject a dye into your arm, allowing them to track how the blood flows in your eye. They’ll take pictures of the dye circulating inside of your eye to determine which vessels are blocked, leaking, or broken.
B Scan Ultrasonography:
It uses ultrasound waves to image the eye when there is no view of the retina due to vitreous haemorrhage.
Frequently Asked Questions (FAQs) about Diabetic Retinopathy
Diabetic retinopathy cannot be fully reversed, but its progression can be slowed or halted with proper management. Early-stage diabetic retinopathy may improve with strict blood sugar, blood pressure, and cholesterol control. However, once significant damage occurs, treatments like laser therapy, anti-VEGF injections, or surgery may be required to prevent further vision loss. Early detection and timely intervention are key to preserving eyesight.
Diabetic retinopathy is detected through a comprehensive eye examination, which includes dilated eye exams, optical coherence tomography (OCT) scans, and fluorescein angiography. During the dilated eye exam, an ophthalmologist examines the retina for abnormal blood vessels, bleeding, or swelling. Regular screenings are crucial for individuals with diabetes, as early detection can prevent severe complications.
In the early stages, diabetic retinopathy may not cause noticeable symptoms. However, the first signs often include blurred vision, difficulty seeing at night, and the appearance of floaters or dark spots in the vision. As the condition progresses, vision may become increasingly distorted, and untreated cases can lead to blindness. Regular eye check-ups help in identifying and managing the condition before severe damage occurs.
To reduce the risk of diabetic retinopathy, maintaining stable blood sugar levels is crucial. Managing blood pressure and cholesterol, following a healthy diet, exercising regularly, and avoiding smoking can help prevent complications. Regular eye exams allow for early detection, and if needed, timely treatment can prevent severe vision loss. Adhering to diabetes management plans as prescribed by a doctor is essential in protecting eye health.
Diabetes-related retinopathy can lead to other serious eye conditions, including diabetic macular edema (DME), cataracts, and glaucoma. DME causes swelling in the retina, leading to vision impairment. Diabetes also increases the risk of cataracts at an earlier age and can contribute to the development of glaucoma, which damages the optic nerve. Managing diabetes effectively reduces the chances of these complications.
A diet rich in antioxidants, omega-3 fatty acids, and essential vitamins can help manage diabetic retinopathy. Foods such as leafy greens, carrots, berries, fatty fish, nuts, seeds, and whole grains support eye health. Omega-3s help reduce inflammation, while vitamins C, E, and zinc promote retinal health. Avoiding excessive sugar, processed foods, and unhealthy fats can also help in preventing further damage.
The best treatment for diabetic retinopathy depends on its severity. In mild cases, controlling blood sugar and maintaining a healthy lifestyle may be enough. For more advanced stages, treatments like laser photocoagulation, anti-VEGF injections, and vitrectomy surgery are available to manage swelling, stop abnormal blood vessel growth, and preserve vision. Regular monitoring and timely intervention are essential for effective treatment and prevention of vision loss.
Proliferative diabetic retinopathy (PDR) is an advanced stage of diabetic retinopathy, a condition that affects the eyes of individuals with diabetes. In PDR, abnormal blood vessels begin to grow on the surface of the retina, the light-sensitive tissue at the back of the eye.
Symptoms of proliferative diabetic retinopathy may include blurred or distorted vision, floaters (spots or dark strings) in the vision, sudden loss of vision, or difficulty seeing colors.
Proliferative diabetic retinopathy develops in individuals with diabetes due to long-term damage to blood vessels in the retina caused by high blood sugar levels. This damage triggers the growth of abnormal blood vessels as the body attempts to compensate for reduced blood flow to the retina.
Proliferative diabetic retinopathy is distinguished from other stages of diabetic retinopathy by the presence of new, fragile blood vessels on the retina’s surface. These vessels can leak blood into the eye, leading to vision loss and other complications if left untreated.
Risk factors associated with the development of proliferative diabetic retinopathy include poorly controlled blood sugar levels, high blood pressure, high cholesterol, long duration of diabetes, and pregnancy in women with diabetes.
Treatment options for proliferative diabetic retinopathy may include laser photocoagulation therapy, intravitreal injections of anti-VEGF drugs, vitrectomy (surgical removal of vitreous gel from the eye), or a combination of these treatments depending on the severity and individual needs of the patient. It’s important for individuals with diabetes to undergo regular eye examinations to detect and manage diabetic retinopathy early to prevent progression to proliferative diabetic retinopathy.
Non-proliferative diabetic retinopathy (NPDR) is an early stage of diabetic retinopathy, where blood vessels in the retina become damaged due to high blood sugar levels.
Early signs and symptoms include blurred vision, difficulty seeing at night, floaters, and mild vision loss. However, NPDR may not always cause noticeable symptoms in the early stages.
NPDR can progress over time, leading to leakage of fluid and blood into the retina, swelling, and thickening of the retina. If untreated, it can lead to vision problems and even blindness.
Factors contributing to NPDR include high blood sugar levels, long duration of diabetes, high blood pressure, high cholesterol, smoking, pregnancy, and genetics.
While NPDR cannot always be prevented, controlling blood sugar, blood pressure, cholesterol, quitting smoking, and regular eye exams can help reduce the risk or delay its progression.
