Glaucoma
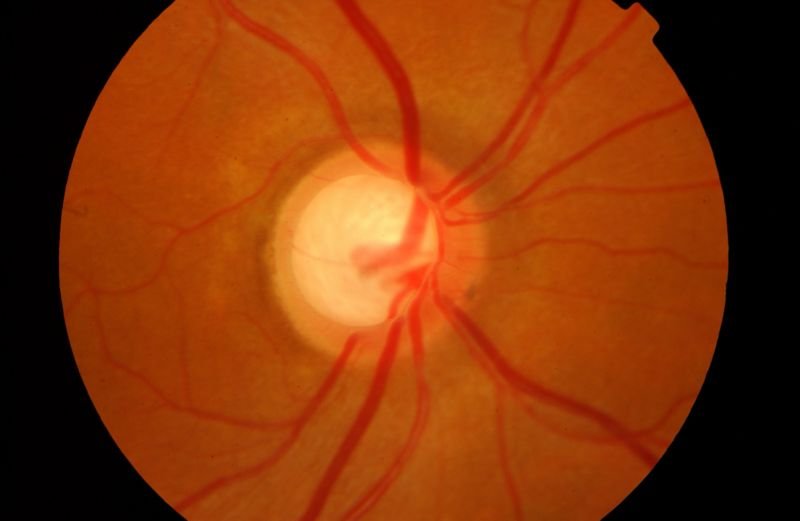
What is Glaucoma?
Glaucoma is a silent thief of sight—one of the leading causes of irreversible blindness worldwide. This progressive eye disease damages the optic nerve due to increased intraocular pressure, leading to gradual vision loss. The most alarming part? It often creeps in without noticeable symptoms until significant damage is done. Understanding glaucoma, its causes, symptoms, and prevention methods can help safeguard your vision.
What Are the Symptoms of Glaucoma?
Glaucoma symptoms vary depending on the type and severity of the condition. While some people may experience gradual vision changes, others may notice sudden and severe symptoms. Below are the warning signs:
1. Loss of Vision
One of the most significant indicators of glaucoma is glaucoma vision deterioration, where blind spots appear in peripheral or central vision.
2. Blurry Vision
Blurred or hazy vision is an early warning sign, especially in angle-closure glaucoma where the pressure spikes suddenly.
3. Persistent Headache
High intraocular pressure can lead to intense headaches, often accompanied by eye pain.
4. Eye Redness
Redness in the eye is another symptom of glaucoma disease, indicating increased intraocular pressure or inflammation.
5. Stomach Upset, Nausea, and Vomiting
In acute cases, sudden pressure spikes can lead to nausea and vomiting, often misattributed to other conditions.
6. Pain in the Eye
Discomfort or severe pain in the eye may indicate phacolytic glaucoma or phacomorphic glaucoma, where lens changes obstruct normal fluid drainage.
7. Early Presbyopia
Difficulty focusing on nearby objects may suggest early onset of eye disorders linked to glaucoma.
Causes of Glaucoma
Several factors contribute to glaucoma. While some are hereditary, others arise due to lifestyle and medical conditions. Glaucoma Causes Included:
1. Build-up of Aqueous Humor Inside the Eye
The eye maintains internal pressure by producing and draining aqueous humor. A blockage in this drainage system can lead to excessive pressure.
2. Genetic Reasons
Family history significantly increases the risk of developing glaucoma symptoms over time.
3. Birth Defects
Congenital defects in the eye’s drainage system can cause childhood glaucoma.
4. Blunt or Chemical Injury
Trauma or exposure to harmful chemicals can disrupt the normal flow of fluids inside the eye.
5. Acute Eye Infection
Certain infections cause inflammation and scarring, leading to glaucoma disease.
6. Blockage by Blood Vessels Inside the Eye
Poor circulation can cause vessel blockages, increasing the risk of glaucoma vision loss.
7. Inflammatory Conditions
Autoimmune diseases like uveitis can trigger secondary glaucoma.
Glaucoma Risk Factors
Are you at risk? Identifying these factors can help with early detection and prevention.
1. Are You Over 60 Years of Age?
Age is a significant risk factor, as the drainage system naturally weakens over time.
2. Have High Internal Eye Pressure?
Elevated intraocular pressure is a primary contributor to glaucoma.
3. Have a Family Member Diagnosed with Glaucoma?
A strong genetic link exists, making family history a key risk factor.
4. Have Certain Medical Conditions?
Diabetes, hypertension, and anemia increase glaucoma susceptibility.
5. Have Thin Corneas?
Thin corneas lead to inaccurate pressure readings, masking high intraocular pressure.
6. Have Extreme Nearsightedness or Farsightedness?
Severe refractive errors alter the eye’s anatomy, increasing glaucoma risk.
7. Have Had Eye Injuries or Surgeries?
Trauma and surgical procedures can alter fluid dynamics inside the eye.
8. Taking Corticosteroids for a Long Time?
Prolonged steroid use can trigger secondary glaucoma
How to Prevent Glaucoma
While glaucoma cannot be completely prevented, early detection and lifestyle changes can slow its progression.
1. Have Eye Checkups Often
Routine exams help detect glaucoma symptoms before irreversible damage occurs.
2. Be Aware of Your Family’s Medical History
If glaucoma runs in your family, regular screenings are essential.
3. Keep Fit and Eat Healthy
A diet rich in leafy greens, omega-3 fatty acids, and antioxidants promotes eye health.
4. Protect Your Eyes While Performing Tasks That Could Cause Injuries
Wearing protective eyewear during sports or hazardous activities prevents trauma-induced glaucoma.
Glaucoma is a serious but manageable condition if diagnosed early. Prioritizing regular eye exams, understanding risk factors, and taking preventive measures can help protect your sight. If you experience any glaucoma symptoms, consult an eye specialist immediately.
Types of Glaucoma
Glaucoma is not a one-size-fits-all disease. It manifests in different forms, each requiring specific treatments.
1. Congenital Glaucoma
2. Primary Open Angle Glaucoma (POAG)
3. Primary Angle Closure Glaucoma (PACG)
4. Secondary Glaucoma
5. Lens Induced Glaucoma
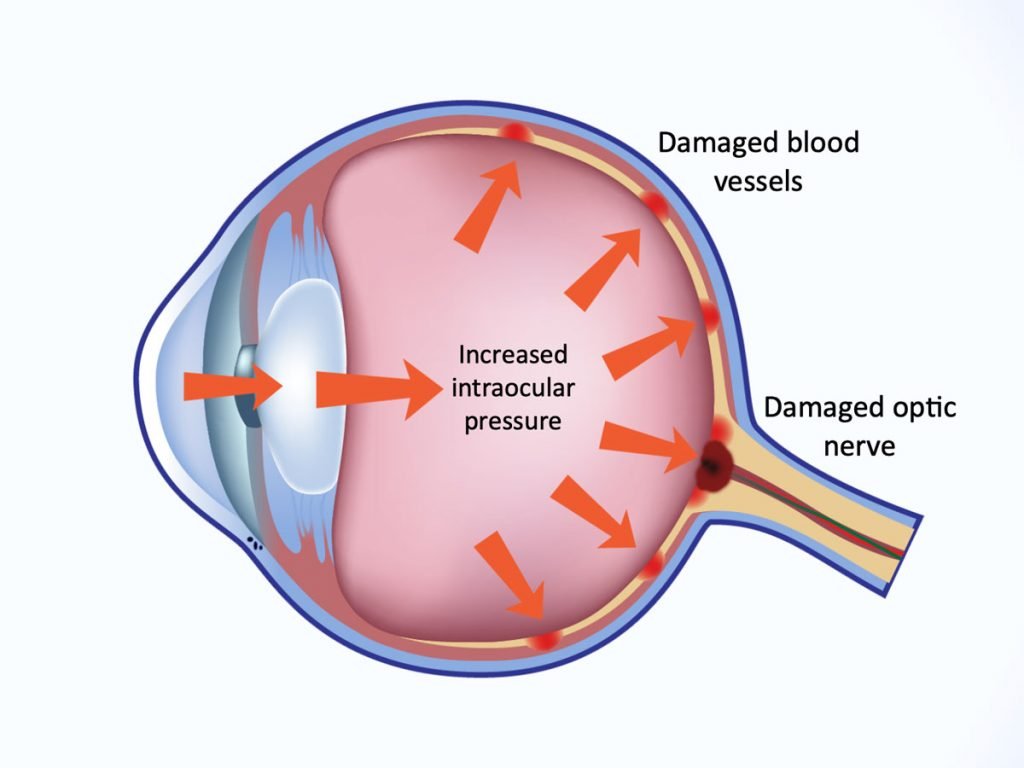
What is Congenital Glaucoma?
Congenital Glaucoma otherwise known as childhood glaucoma, infantile glaucoma or pediatric glaucoma is found to occur in babies and small children ( < 3 years of age). It is a rare condition but could result in a permanent loss of vision.
Congenital Glaucoma Symptoms
The symptoms and signs of childhood glaucoma include:
• Triad
• Overflow of tears onto the face (Epiphora)
• Involuntary twitching of the eye (Blepharospasm)
• Sensitivity towards the light (Photosensitivity)
• Enlargement of the eyes (Buphthalmos)
• Hazy cornea
• Closing of the eyelid
• Redness of the eye
Congenital Glaucoma Causes
• Build-up of aqueous humor inside the eye
• Genetic reasons
• Birth defects in ocular angle
• Underdeveloped cells, tissues
Congenital Glaucoma Risk Factors
From what is known the risk factors could be
• Family’s medical history
• Gender
Congenital Glaucoma Prevention
Even though congenital glaucoma cannot be fully prevented, complete vision loss could be prevented when diagnosed early. Some of the best ways to ensure we catch congenital glaucoma early are
• To have eye checkups often
• To be aware of your family’s medical history
Two types of glaucoma are:
• Primary Congenital Glaucoma:
which means that the condition is not a result of another condition at birth.
• Secondary Congenital Glaucoma:
which means that the condition is a result of another condition at birth. For example, tumour, infections, etc.
Congenital Glaucoma Diagnosis
The doctor will conduct a thorough eye exam on the child. To make it easy for the doctor to visualize a small eye, the examination would be conducted in an operating room. The child would be under anaesthesia during the procedure. The doctor will then measure the child’s intraocular pressure and carefully examine every part of the child’s eye. The doctor would make a diagnosis only after considering all the symptoms, ruling out other ailments that caused the child’s problems.

Congenital Glaucoma Treatment
For congenital glaucoma treatment, once it is diagnosed, doctors almost always opt to treat it by surgery. Since it is risky for infants to be under anaesthesia, doctors like to perform the congenital glaucoma surgery immediately after the diagnosis is made. If both the eyes are found to have congenital glaucoma, the doctors prefer performing the surgery on both eyes at once.
In case the doctors are not able to perform immediately, they may prescribe oral medications and eye drops or a combination of both to help in maintaining, reducing the eye pressure.
Sometimes, microsurgery could become an option. To reduce the eye pressure, the doctor creates a new channel to ease the flow of the fluid. A valve or tube may be implanted to drain the fluid. Laser surgery could also be used if other methods do not work. Lasers would be used to lessen fluid production.
Even though congenital glaucoma is not completely reversible, it could be controlled and a complete vision loss could be prevented. You could treat it before it worsens. If your child shows any of these symptoms or is diagnosed with congenital glaucoma get in touch with us today to be treated by some of the safest hands! Book an appointment now for Glaucoma Treatment and other Eye Treatment.
Primary Open Angle Glaucoma (POAG)
Glaucoma is a well-known eye disease that damages the optic nerves and may eventually result in complete blindness in the worst cases. It affects a large number of people around the world and is the leading cause of eye blindness. Under the term ‘glaucoma,’ open angle glaucoma is the most common type. It leads to an increase in pressure inside the eyes, which gradually does damage to the optic nerves. It is not possible to completely cure this eye condition, but it can be prevented from progressing. Since open angle glaucoma is an eye disease that may cost you your vision, it is important you get your eyes checked regularly. It will allow you to diagnose the disease as early as possible. This article will help you understand everything you need to know about this eye condition, including its symptoms, risk factors, and treatment.
Closed vs Open Angle Glaucoma
Before we get into the symptoms and treatment for open angle glaucoma, let us first understand the difference between open and closed angle glaucoma. The part of our eyes between the cornea and the lens is made up of watery fluid called aqueous humor. This fluid is constantly being produced and drained out through: • the trabecular meshwork • the uveoscleral outflow The primary difference between open and closed angle glaucoma depends on which of the two drainage paths is damaged. In open angle glaucoma, the trabecular meshwork resists fluid outflow, and in the case of closed angle glaucoma, both trabecular meshwork and uveoscleral drain get blocked.
Symptoms of Open Angle Glaucoma
In the early stages, glaucoma does not show any symptoms. It gradually progresses and can cause damage to your vision before you know it. However, see an eye specialist if you experience any of these open angle glaucoma symptoms:
• bulging or swollen cornea
• reduced peripheral vision
• eye redness
• nausea
• pupil dilation that doesn’t change with the brightness of the light
It is important to remember that absence of these symptoms does not mean that one cannot contract open angle glaucoma.
Risk Factors of Glaucoma
More than 80% of glaucoma cases are of open angle glaucoma. Risk factors for this eye condition include:
• Family history of glaucoma
• High IOP (intraocular pressure)
• Tumor
• Inflammation
• Low blood pressure
• Old age
• Nearsightedness
Open Angle Glaucoma Diagnosis
If you have a high IOP, you may contract open angle glaucoma. But it is not a sure sign. If you want to determine whether you have open angle glaucoma, you must go through a comprehensive eye examination. Some of the eye test that your eye doctor will use are:
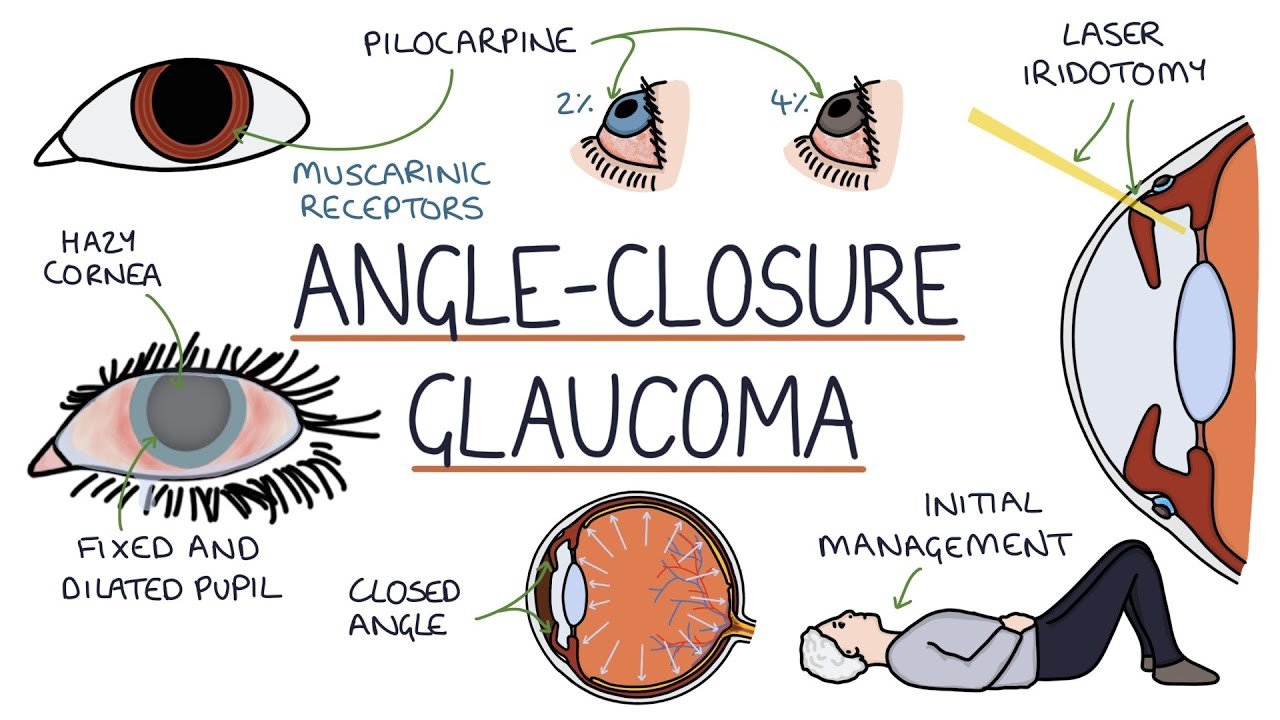
• Visual Acuity Test:
This test is performed using an eye chart to assess the ability of the eyes to focus and discern objects.
• Visual Field Test:
This test helps check peripheral vision.
• Dilated Eye Exam:
It is the most important eye examination to diagnose open angle glaucoma. Eye drops are given to dilate the pupils, which helps the eye specialist to look into the optic nerves and the retina. They make use of a special instrument called the ophthalmoscope. The whole process is painless.
• Tonometry:
In this test, the eye doctor applies numbing drops to the eyes and uses a certain instrument to measure the pressure near the cornea. This test is also quite painless except for the slight sting that you might feel when the eye drop is applied.
• Pachymetry:
After the application of numbing drops to your eyes, the doctor uses a machine that produces ultrasound waves. It helps them to measure the thickness of the cornea.
• Gonioscopy:
To Check whether angle of Anterior chamber is open or closed to determine type of glaucoma.
Primary Angle Closure Glaucoma (PACG)
Glaucoma is an eye condition which causes damage to optic nerve. It is one of the leading causes of blindness in adults across the world. Therefore, it is important to have the right knowledge about this disease so you can get the right treatment at the right time. There are multiple eye diseases that fall under the name of ‘Glaucoma.’ Over 90% of the cases of glaucoma are found to be open angle glaucoma. But there is another form of glaucoma that many people do not know about—Close angle glaucoma. It is a type of condition that, if left untreated, may ultimately lead to blindness. This article will help you understand everything you need to know about this eye disease, including its types, symptoms about Closed angle glaucoma treatment.
What is Closed Angle Glaucoma?
Closed angle glaucoma refers to a condition where the pressure inside the eyes becomes a lot higher than usual. The pressure gets built up because the fluid is not able to flow out as it should. This fluid is usually produced at the rear of the eye, behind the iris. It flows through the pupil into the front part of the eye. It then goes through a number of channels known as trabecular meshwork and, after that, into the veins of the sclera (the white part of the eye). However, in the case of closed angle glaucoma, the trabecular meshwork gets damaged or obstructed. The fluid cannot flow easily through the pathway or get completely blocked. This backup of fluid leads to an increase in pressure within the eyeballs.
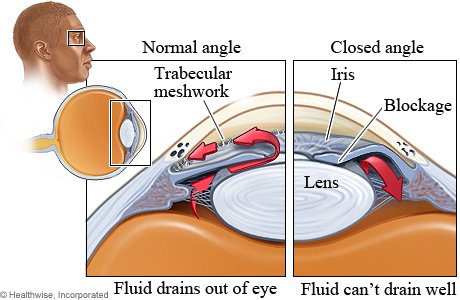
Types of Closed Angle Glaucoma
Closed angle glaucoma can be broadly divided into two categories—Primary closed angle glaucoma and Secondary closed angle glaucoma. Let us understand them both briefly:
• Primary Closed Angle Glaucoma
In this type of closed angle glaucoma, the structure of our eyes becomes such that the iris may get pressed against the trabecular meshwork. This may happen because of the following reasons:
1. The angle between the cornea and the iris is very narrow.
2. The eye lens is thick and pushes the iris forward.
3. The eyeball is relatively small when measured from front to back.
4. The iris is thinner and makes it fold into the angle
. Secondary Closed Angle Glaucoma
Secondary closed angle glaucoma is an eye condition which causes changes in the eye that basically force the iris against the trabecular meshwork. These are some of the underlying conditions:
1. Inflammation
2. Diabetes
3. Eye injury
4. Tumour
5. Advanced cataract (clouding of the eye lenses)
Closed angle glaucoma may also be described as either acute or chronic. Acute cases are quite common compared to chronic ones and may occur suddenly. In contrast, chronic closed angle glaucoma develops slowly, and its symptoms are hard to spot.
Symptoms of Closed Angle Glaucoma
In case you are suffering from acute closed angle glaucoma, you may experience a sudden onset of more than one of the following symptoms:
1. Blurred vision
2. Severe eye pain
3. Eye redness, hardness, and tenderness
4. Feeling nauseated or wanting to vomit
5. Visibility of white halos around objects
You may get prone to closed angle glaucoma if your pupils stay dilated. For instance, when you are under stress, taking certain drugs, or when you are in a darkened room. If any of these symptoms occur to you, it would be best to see an eye specialist right away, especially in the case of acute closed angle glaucoma. The symptoms of chronic closed angle glaucoma are subtler in nature. One may not be able to notice any changes at first. However, as the condition progresses, one may realize that their sight is deteriorating, and they are losing the edges of their field of vision. In this eye condition, one may even experience eye pain and redness but not as severe as in the case of acute closed angle glaucoma.
Who is at Risk of Contracting Closed Angle Glaucoma?
There is a greater risk of closed angle glaucoma if you are:
1. Farsighted
2. Older than 40 years, especially if you are between 60 and 70 years old.
3. If you have a sibling or a close relative with the disease of southeast Asian origin.
Treatment for Closed Angle Glaucoma
There are many ways to treat closed angle glaucoma. One may go for medication or surgery, or both as advised by the eye specialist. Let us take a look at both these treatment alternatives.
Prevent Closed Angle Glaucoma with the Best Treatment
In case you have a family history of this eye condition, you should get your eyes checked regularly. Also, see the eye specialist if you face any of the symptoms mentioned. Closed angle glaucoma is an eye disease which, in worst cases, may take away the light from someone’s eyes. Therefore, it is essential to get the best possible treatment available.
Medication
If your eye doctor suggests you take medication for closed angle glaucoma, you may be required to take multiple drugs, including:
1. Painkillers to reduce the pain in the eyes.
2. Drugs to treat vomiting and nausea.
3. Acetazolamide to reduce the fluid in the eyes.
4. Pilocarpine to open the angle between the cornea and iris.
5. Steroids to reduce inflammation.
6. Beta-blockers to reduce fluid production inside the eyes.
Surgery
After the pressure in the eyes reduces, you may require further treatment to prevent the pressure from rising. There are two types of surgeries to address this issue:
1. Peripheral Iridotomy: It is a laser surgery in which very small drainage holes in the iris. This method is used to treat both chronic and acute closed angle glaucoma.
2. Surgical Iridectomy: In this type of surgical treatment, the doctor makes a triangular opening in the iris.
What is Secondary Glaucoma?
Let’s try to understand this a little better. The frontal region of the eye, between the cornea and lens, is filled with a fluid called aqueous humor. This liquid is regularly drained and produced and maintains a constant balance. The aqueous humor constantly drains out through the trabecular meshwork or the uveoscleral outflow. Blockage in either of these can cause eye pressure to increase, which in turn damages the optic nerve can be categorized as secondary glaucoma. Similar to primary glaucoma, secondary glaucoma can affect one or both eyes.
Depending on what pathway is blocked, secondary glaucoma can be categorized into secondary open-angle glaucoma or secondary angle-closure glaucoma. In the former, the trabecular meshwork resists the liquid from flowing freely whereas, in the latter, both the pathways get blocked, mostly caused by a damaged iris blocking the pathways. Both of these are caused by the angle of the iris with the cornea, depending on this either of the pathways could be blocked.
Symptoms of Secondary Glaucoma
• Patchy blind spots in your peripheral vision
• Severe headache
• Pain in the eyes
• Nausea and vomiting
• Visible halos around lights
• Redness of the eyes
Once these symptoms appear, immediate action should be taken as secondary glaucoma causes blindness if left untreated. Now that we know what secondary glaucoma is, let’s look into what causes secondary glaucoma to appear in the first place.
Secondary Glaucoma Causes
• Usage of steroids
• Diabetes
• Eye injury – trauma or blow to the eye
• Eye inflammation
• Advanced stages of cataract
Prevention of Secondary Glaucoma
The best way to prevent secondary glaucoma is
• By taking regular eye exams and getting your eyes checked
• Maintain health by keeping the body active – regular exercise helps keep eye pressure in control
• Avoid blows to the eyes by wearing protective eye gear during extreme sports
Multiple types of Secondary Glaucoma such as
• Exfoliative Glaucoma– caused by flakes of the outer layer of the eye which can clog the drainage system.
• Neovascular Glaucoma– caused by abnormal growth of blood vessels in the eye, often associated with diabetes
• Pigmentary Glaucoma– caused by the breaking away of pigments of the iris which break into the clear liquid of the eye.
• Traumatic Glaucoma– caused due to eye injury
• Uveitic Glaucoma– caused by the swelling of the uvea
• Congenital Glaucoma
Diagnosis of secondary glaucoma
The diagnosis of secondary glaucoma generally includes a simple procedure which begins with a dilution of the eyes post which the optometrist will check your optic nerve for signs of glaucoma and most often takes pictures to compare during your next visit.
Other tests for secondary glaucoma include,
• Tonometry– a test to check the pressure of the eye.
• Visual field test– a test to check your peripheral vision.
• Visual acuity test– to check vision at various distances.
• Gonioscopy– an instrument based test to check the front part of the eye.
• Ophthalmoscopy– a test to check the interior of the eye using a special instrument.
Treatment of secondary glaucoma
Secondary glaucoma treatment often includes attempting to bring the eye pressure down through multiple methods. Quite often the underlying issues are also targeted to reduce their impact on the eyes. But the most common treatment options for secondary glaucoma include.
• Eye Drops   
• Oral Medication   
• Laser   
• Surgery
Each of these methods is used to ensure that the eye pressure comes down until the underlying issues such as diabetes or injuries to the eye are dealt with.
What is Lens Induced Glaucoma?
With the damage to the optic nerve, lens induced glaucoma is caused by the leakage of lens material in one’s eye. The leakage can typically be from a dense or late cataract. This type of glaucoma can happen in open-angle or angle-closure forms. The lens induced glaucoma needs more attention and care, as unlike other glaucoma, this cannot be ignored, and when left untreated it can lead to loss of peripheral vision
Lens Induced Glaucoma Symptoms
There are a set of signs that indicate Lens induced glaucoma. Very common ones include:
• Pain in the eyes
• Loss of sight
• Redness
• Fading of visual clarity
A few other symptoms that could be experience by others include:
• Clouding of the eyes
• Tearing
• Corneal edema
• Photophobia (a discomfort in the eyes that is felt because of the contact with high levels of light or by the occurrence of physical sensitivity within the eyes)
Lens Induced Glaucoma Causes
Angle-closure
• Due to swelling of lens (phacomorphic glaucoma)
• Due to discoloration of lens (ectopia lentis)
Open angle
• Due to the leakage of lens proteins through the capsule of mature/ hypermature cataract (phacolytic glaucoma)
• Due to the obstruction of the meshwork after cataract treatment.
• Due to capsulotomy
• Due to ocular trauma caused by fragments of lens (lens-particle glaucoma)
• Due to hypersensitivity to own lens protein after a cataract surgery (phacoantigenic glaucoma)
Lens induced glaucoma is caused by the leakage of lens materials through the capsule of a developed cataract. The leakage of lens material from one’s lens can get into the drainage system of the eye, which leads to obstacles of outflow of the usual aqueous liquid within the eye. This can cause a build-up of aqueous inside the eye, in-turn increasing eye pressure and damage to the optic nerve.
Prevention measures for Lens Induced Glaucoma
If taken care properly, prevention of Lens induced glaucoma is possible. Some of the prevention measures include:
• Regular eye and diabetic examination
• Family health history plays a major role. Understand and examine the same. Glaucoma can be a hereditary
• Build a regular and safe exercise routine
• Wear eye protection
• Take only prescribed eye drops
Different types of Lens Induced Glaucoma are
• Phacolytic glaucoma.
• Phacomorphic glaucoma
• Lens particle glaucoma.
• Phacotopic glaucoma.
• Phacoanaphylatic uveitis with secondary glaucoma.
Lens induced glaucoma Diagnosis
Diagnosis of each type of the Lens induced glaucoma has different process:
• When it comes to Phacomorphic glaucoma, it is diagnosed by eye pain, decreased vision, formation of mature cataract and intraocular pressure in the eye.
• Ectopia lentis varies from person to person based on the state of their lens, but when it is dislocated, it leads in angle-closure and blockage in the pupillary. Usually people will undergo pain in their eyes, decreased visual clarity and face difficulties in placing things especially near vision.
• In Phacolytic glaucoma, the patient will undergo pain in the eye with photophobia, decrease in vision and high conjunctival hyperemia. Diagnosis of such glaucoma is done with a prominent cell or white particle in one’s anterior chamber, corneal edema, increase in intraocular pressure and the sign of mature cataract.
• In lens-particle glaucoma, the signs occur usually after a few days or weeks or even a month or year later. An accurate diagnosis includes a surgery or trauma in the past. Elevated intraocular elements and signs of cortical lens particles in the anterior chamber are few clinical findings of these.
• Clinical findings for Phacoantigenic glaucoma include keratic precipitates, anterior chamber flare response and residue in the lens materials. This kind of glaucoma occurs between 1 & 14 days of a cataract surgery.
Lens Induced Glaucoma Treatment
Lens induced glaucoma treatment requires immediate attention, and treating it promptly is of utmost importance, as it might lead to serious consequence if left unnoticed, including intractable glaucoma owing to peripheral anterior synechiae triggered by continual inflammation. Additionally, this might lead to the development of pupillary membrane and eventually leading to a blockage in ones pupillary. There is a possibility of permanent damage to the aqueous outflow channels if the lens particles are not removed from the eye. However, the treatment differs on the seriousness of the dislocation of the pupillary block. When there is subluxation without a pupillary block, treatment with intraocular pressure would be advised to follow. When there is a serious pupillary block that is present, a laser iridectomy is suggested. When there is a complete anterior dislocation, the treatment would be to remove the lens.
FAQ (Frequently Questioned Answers)
Glaucoma is a common eye disease that leads to the damage of the optic nerve. This damage to the optic nerve, which transmits information from the eyes to the brain, results in vision loss. If not treated properly, visual loss may be temporary or permanent. A change in the eye’s internal fluid pressure, also known as intraocular pressure (IOP), is the most common cause of Glaucoma.
Glaucoma affects around 70 million individuals globally. In 2020, glaucoma disease will affect over 80 million individuals worldwide, with the number anticipated to rise to over 111 million by 2040. Glaucoma is the main cause of irreversible blindness, accounting for 12.3% of all blindness worldwide.
Below we have given an insight into both these two types of glaucoma:
- Open angle glaucoma: The most prevalent type of glaucoma is open-angle glaucoma. It has no symptoms at first; however, side (peripheral) vision is lost at some time, and without treatment, a person can become completely blind.
- Closed angle glaucoma: Angle-closure glaucoma, also known as closed angle glaucoma, is a less prevalent kind of glaucoma. It happens when the drainage system in the eye gets fully obstructed, causing the pressure inside the eye to rapidly rise.
Glaucoma can be inherited in some cases, and many experts around the world are researching genes and their effects on the disease. Glaucoma is not always hereditary, and the circumstances that lead to the beginning of the illness are yet to be fully understood.
The measurement of eye pressure is in millimetres of mercury (mm Hg). The typical range for eye pressure is 12-22 mm Hg, while pressures more than 22 mm Hg are considered abnormal. Glaucoma is not caused by high eye pressure alone. It is, nonetheless, a considerable risk factor. Individuals with high eye pressure should get comprehensive eye exams by an eye care specialist on a regular basis to screen for signs of glaucoma.
Unfortunately, there is no glaucoma cure, and the vision loss resulted due to it is irreversible. If someone suffers from open-angle glaucoma, it has to be monitored for the rest of their life.
However, it is possible to slow down or stop additional vision loss using the medication, laser treatment, and surgery. The most important thing to remember here is that the first step in preserving your vision is to get a diagnosis. So, never ignore it if you experience any discomfort in your vision.
When the classic optic nerve and vision alterations occur, glaucoma disease is diagnosed, usually with raised eye pressure but rarely with normal pressure. Ocular hypertension occurs when the intraocular pressure is higher than usual, but the person does not display indications of glaucoma.
Generally, chronic forms of glaucoma, like primary open angle glaucoma, do not lead to headaches. However, acute forms when the eye pressure increases, can cause headaches.
Some of the closed angle glaucoma risk factors include:
- Age over 55.
- Increase eye pressure
- The thin cornea at the centre
- Family history of glaucoma
- This eye condition gradually causes vision to get worse. If left untreated, closed angle glaucoma may lead to blindness in the worst-case scenario.
- Common causes of secondary glaucoma include eye trauma, certain medications such as corticosteroids, uveitis (inflammation of the middle layer of the eye), neovascularization (abnormal formation of new blood vessels), and conditions like pigment dispersion syndrome or pseudoexfoliation syndrome.
- Treatment for secondary glaucoma depends on the underlying cause and severity of the condition. It may include medications such as eye drops to lower intraocular pressure, laser therapy (laser trabeculoplasty) to improve drainage of aqueous humor, conventional surgery (trabeculectomy) to create a new drainage channel, or minimally invasive procedures like trabecular micro-bypass stents. The choice of treatment is determined by the ophthalmologist after careful evaluation of the individual case. Regular follow-up appointments are crucial to monitor the condition and adjust treatment as needed.
If not treated adequately in the early stages of glaucoma disease, it can severely affect the peripheral vision, leading to a condition known as ‘tunnel vision. Tunnel vision eliminates your ‘side vision,’ limiting your field of view to images in your central vision or straight ahead.
If you feel that you are experiencing any glaucoma symptoms, it can be detected during a full dilated eye examination. The examination is straightforward and painless: your doctor will dilate (widen) your pupil with eye drops before checking your eyes for glaucoma and other eye issues.
A visual field test is included in the exam to examine your side vision. People with a family history of glaucoma should have their eye pressure and optic nerves tested frequently since they are at a higher risk of developing the condition.
Lens-Induced Glaucoma occurs when the eye’s natural lens triggers increased pressure within the eye, leading to optic nerve damage and vision loss. This condition typically arises when the natural lens becomes dislocated, causing obstruction in the drainage system of the eye, known as the trabecular meshwork, resulting in elevated intraocular pressure (IOP).
Lens-Induced Glaucoma is diagnosed through a comprehensive eye examination, which includes measuring intraocular pressure, assessing the drainage angles of the eye using gonioscopy, and evaluating the optic nerve for signs of damage. Additionally, imaging tests such as optical coherence tomography (OCT) may be employed to provide detailed images of the optic nerve and the surrounding structures.
Symptoms of Lens-Induced Glaucoma may include sudden onset of eye pain, blurred vision, halos around lights, redness in the eye, nausea, and vomiting. However, it’s important to note that some individuals may not experience any noticeable symptoms until the condition has progressed significantly, highlighting the importance of regular eye examinations.
A major risk factor of primary open angle glaucoma is age. As we humans get older, our drainage pathway of the eyes starts to function less efficiently, and the eye pressure keeps increasing.
An angle closure glaucoma may rise within a few hours. It occurs when the eye fluid is not able to drain out.
Yes, there is a high chance of you contracting closed angle glaucoma if any of your close family members have it.
- Secondary glaucoma is a condition characterised by increased intraocular pressure (IOP) due to identifiable underlying causes, whereas primary glaucoma occurs without any identifiable cause. In secondary glaucoma, the elevated pressure within the eye is a result of a pre-existing condition or a complication of another eye disease, distinguishing it from primary glaucoma.
- Symptoms of secondary glaucoma may include blurred vision, severe eye pain, headache, nausea, vomiting, and halos around lights. Diagnosis typically involves a comprehensive eye examination, measurement of intraocular pressure, examination of the optic nerve, and imaging tests such as optical coherence tomography (OCT) or visual field testing.
